Gut Dysbiosis: Causes, Symptoms & What It Means
Gut dysbiosis means an unbalanced gut microbiome. Learn what causes it, which health conditions it drives, and how doctors test for it.
Your gut is home to trillions of microorganisms — bacteria, fungi, viruses — that keep your digestion, immunity, and even your mood running smoothly. When that community falls out of balance, healthcare providers call it gut dysbiosis. And the consequences reach far beyond an upset stomach.
Understanding gut dysbiosis matters because it quietly underpins conditions ranging from inflammatory bowel disease to cardiovascular risk. This article breaks down exactly what dysbiosis is, what disrupts your microbiome, which health conditions it connects to, and how doctors actually test for it.
What Is Gut Dysbiosis?
Gut dysbiosis is the clinical term for an unbalanced or unhealthy gut microbiome. It typically involves three overlapping problems:
- A loss or deficit of beneficial bacteria — the helpful microbes that protect and nourish your gut lining.
- Overgrowth of potentially pathogenic bacteria — harmful or invasive types that take advantage of the gap.
- A breakdown of the healthy overall balance — where no single disruption stays isolated for long.
These three factors are interconnected. When beneficial bacteria decline, your gut loses its natural defenses. Pathogenic types seize the opportunity, crowd out remaining healthy microbes, and destabilize the entire ecosystem. What begins as one imbalance quickly cascades into all three.
Think of your gut like a garden. A thriving garden resists weeds because healthy plants compete aggressively for space, water, and nutrients. Remove those healthy plants, and weeds don't just appear — they dominate.
What Disrupts Your Gut Microbiome?
Four main environmental factors shape the health of your gut microbiome on a daily basis: diet, chemical exposure, microbial balance, and bowel motility. Each one can push your microbiome toward or away from dysbiosis.
Diet
A diverse microbiome needs diverse plant fiber. Different microbial species thrive on different whole foods. When they break down plant fibers, they produce short-chain fatty acids and other compounds that nourish the gut lining and lower the internal pH — an environment where beneficial microbes flourish.
A diet dominated by sugar and saturated fat tips the balance the other way. Processed foods remove the fiber and micronutrients your microbiome depends on, while introducing additives and preservatives that can actively harm beneficial bacterial populations.
Chemical Exposure
Alcohol, tobacco smoke, environmental pollutants, and certain medications can poison your microbiome. Antibiotics are the most well-known example — they eliminate harmful bacteria but wipe out beneficial strains in the process. Acid-blocking medications shift gut pH in ways that alter microbial composition.
Short-term or necessary chemical exposure — a prescribed course of antibiotics, for example — is something a healthy microbiome can usually recover from. Chronic exposure is far more damaging. Frequent alcohol use or long-term medication use can permanently suppress certain microbial populations.

Microbial Balance
Healthy microorganisms actively support one another. Some species break down compounds that feed neighbouring species. Others produce byproducts that adjust the acidity of the gut environment in ways that benefit the broader community — much like plants cross-pollinating or enriching soil for each other.
When that cooperative network breaks down, invasive species face no competition. Without the checks provided by a diverse microbial community, opportunistic organisms consume available resources and spread beyond their normal territory. The garden fills with weeds.
Bowel Motility
Motility — the regular movement of your bowels — acts as a reset mechanism for your gut microbiome. As food and waste travel through your colon, microorganisms help break down undigested material into absorbable nutrients before leaving the body with your stool.
Speed matters here. If transit is too fast, microbes don't have time to do their jobs or establish healthy populations. If transit is too slow, bacteria can overfeed, overgrow, and migrate into areas where they don't belong — which is precisely how small intestinal bacterial overgrowth (SIBO) can develop.
Health Conditions Linked to Gut Dysbiosis
Gut dysbiosis is not just a digestive issue. Research increasingly links it to conditions across the body. Some are directly caused by dysbiosis; others are indirectly related through complex inflammatory and immune pathways.
Conditions Directly Related to Gut Dysbiosis
Gut infections are a direct consequence of a weakened microbial defense. Invasive pathogens that might otherwise be kept in check by a healthy microbiome can cause diarrhea, inflammation (colitis), and damage to the gut lining. In severe cases, some pathogens breach the gut barrier entirely and enter the bloodstream.
SIBO (Small Intestinal Bacterial Overgrowth) is essentially dysbiosis localized to the small intestine. Certain bacterial strains overgrow, consuming resources and producing excessive byproducts that cause bloating, pain, and malabsorption. In some cases, bacteria migrate from the large intestine into the small intestine — a process often driven by sluggish gut motility.
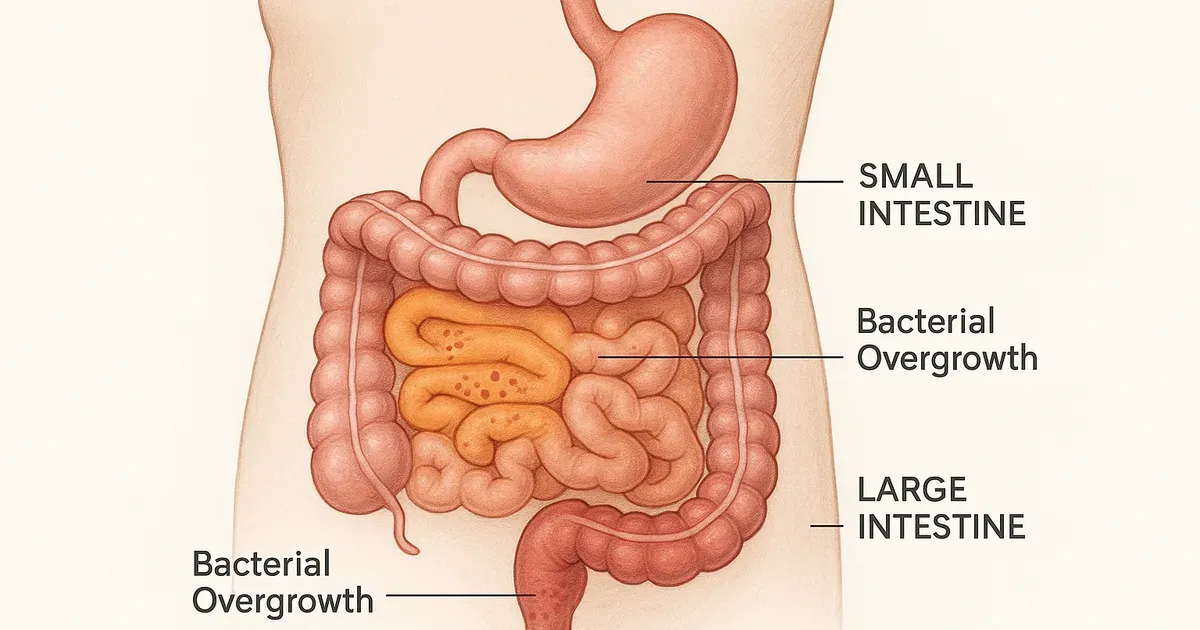
Inflammatory Bowel Disease (IBD) — which includes ulcerative colitis, microscopic colitis, and Crohn's disease — has a well-established relationship with gut dysbiosis. Dysbiosis is one of the diagnostic criteria for IBD. Researchers are still determining which comes first, but the evidence is clear: each condition worsens the other in a reinforcing cycle.
Atherosclerosis illustrates how gut dysbiosis can drive cardiovascular disease. Certain undesirable gut bacteria produce a compound called trimethylamine N-oxide (TMAO) as a metabolic byproduct. TMAO accumulates in arteries and contributes to their hardening. Cardiac blood tests now screen for TMAO as part of coronary artery disease (CAD) risk assessment.
Conditions with Indirect Links
Beyond these direct connections, ongoing research is exploring gut dysbiosis as a contributing factor in a wide range of conditions — including metabolic disorders, mental health conditions, autoimmune diseases, and more. The gut-brain axis, which connects gut microbial activity to neurological function, is one of the most active areas of current investigation.
Common Symptoms of Gut Dysbiosis
Gut dysbiosis rarely announces itself with a single obvious symptom. The signs tend to be varied and easy to attribute to other causes, which is part of what makes it difficult to identify without clinical investigation.
Common symptoms associated with an imbalanced gut microbiome include:
- Bloating and excess gas — a frequent result of bacterial overgrowth and abnormal fermentation
- Diarrhea or constipation — both can reflect disrupted microbial activity and altered motility
- Abdominal discomfort or cramping
- Food intolerances that seem to worsen over time
- Fatigue and low energy — potentially linked to impaired nutrient absorption
- Brain fog and difficulty concentrating — consistent with gut-brain axis disruption
- Frequent infections or weakened immunity — reflecting the gut's central role in immune defense
No single symptom confirms dysbiosis. These complaints are common to many conditions, which is why clinical testing and professional assessment matter.

How Is Gut Dysbiosis Tested and Diagnosed?
Commercial gut microbiome test kits are widely available — you send a stool sample to a lab and receive a report on your microbial composition. However, clinical healthcare providers generally do not recommend these tests for diagnostic purposes.
The reason is straightforward: science has not yet progressed far enough to translate a microbiome composition report into reliable, personalised health guidance. Research is advancing rapidly, but the complexity of the microbiome means consumer-level tests cannot yet offer clinically actionable insights.
What Doctors Actually Test For
Healthcare providers focus on diagnosing specific conditions rather than measuring dysbiosis as a standalone finding. The following tests are used in clinical practice:
- Blood tests — can detect markers of infection, inflammation, or metabolic byproducts like TMAO
- Stool tests — used to identify specific pathogens, parasites, or signs of gut inflammation
- Breath tests — a key tool for diagnosing SIBO; different bacteria produce distinct gases (like hydrogen or methane) that are detectable in exhaled breath after consuming a specific sugar solution
A breath test is non-invasive and clinically validated for detecting bacterial overgrowth in the small intestine. It remains one of the most useful diagnostic tools for conditions tied to gut dysbiosis.
If you suspect a problem with your gut microbiome, the most productive first step is a conversation with your doctor — who can order the appropriate tests based on your specific symptoms and history.
The Bottom Line on Gut Dysbiosis
Gut dysbiosis describes a breakdown in the balance of your gut microbiome — a loss of beneficial bacteria, an overgrowth of harmful types, and a disruption to the ecological balance your digestive health depends on. Diet, chemical exposure, microbial interdependence, and bowel motility all play direct roles in whether your microbiome thrives or falters.
The health consequences of dysbiosis extend well beyond digestion — touching cardiovascular health, immune function, and neurological wellbeing. While commercial testing kits are not yet clinically useful, doctors can test for specific related conditions using blood, stool, and breath tests.
A diverse, plant-rich diet, minimal unnecessary medication use, and attention to bowel regularity are among the most evidence-supported strategies for maintaining a healthy gut microbiome. If symptoms persist, clinical assessment is always the right next step.
