Hormonal Acne and the Gut-Skin Axis: A Complete Guide to Adult Breakouts, Skin Purging and Clear Skin
Adult acne is rarely just a skincare problem. This guide explains the gut-skin axis, how hormones trigger breakouts, and what an evidence-based inside-out approach to clear skin actually looks like.

You followed every skincare rule. You double-cleanse, use SPF, and have a drawer full of serums. And yet, here you are — jawline congested, chin sore, forehead flaring up before your period like clockwork.
Adult acne affects around 50% of women in their 20s, and up to 25% of women in their 40s. If your skin is still breaking out well past adolescence, it is almost never just a hygiene or skincare problem. It is usually a signal — from your hormones, your gut, or both — that something internal needs attention.
This guide covers what science currently knows about the gut-skin axis, why hormones drive breakouts, and what an evidence-based inside-out approach to clear skin actually looks like.
What Is the Gut-Skin Axis?
The gut-skin axis is the two-way communication network between your gastrointestinal system and your skin. Researchers have known for decades that gut and skin conditions tend to cluster together: people with IBS have higher rates of rosacea and acne; people with inflammatory skin conditions often have disrupted gut microbiomes.
The mechanisms are still being mapped, but several pathways are well-established:
Systemic inflammation. When the gut barrier is compromised — a state sometimes called increased intestinal permeability — bacterial fragments can enter the bloodstream and trigger a low-grade inflammatory response throughout the body. Skin, as the largest organ, is often an early casualty.
The microbiome and immune signalling. Around 70% of the immune system lives in the gut. The composition of your gut microbiome directly influences immune responses elsewhere in the body, including the skin. Imbalanced gut bacteria (dysbiosis) can tip the immune system toward chronic inflammatory activity.
Hormonal metabolism. The gut microbiome helps metabolise and regulate oestrogen and other hormones. An imbalanced microbiome can cause hormones to be reabsorbed rather than excreted, contributing to the hormonal fluctuations that drive acne.
The gut-brain-skin connection. Stress activates the gut-brain axis, alters gut permeability, and triggers cortisol and androgen spikes — all of which feed directly into acne pathways.
Why Hormones Cause Acne
Hormonal acne is driven primarily by androgens — testosterone and its derivatives — which stimulate sebaceous glands to produce more sebum (skin oil). Excess sebum, combined with dead skin cells and the bacteria C. acnes, creates the conditions for blocked pores and breakouts.
Hormonal fluctuations that trigger acne include:
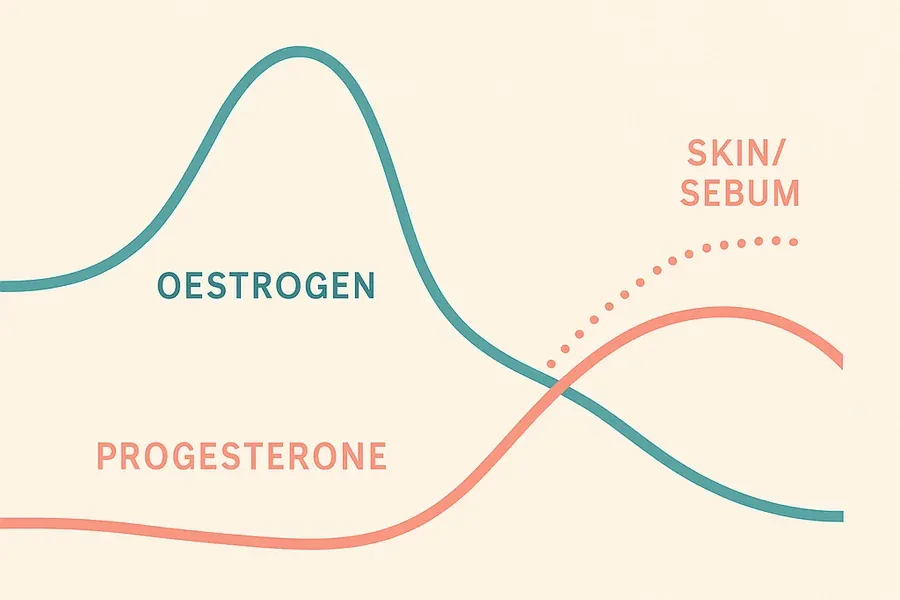
- The menstrual cycle — progesterone rises in the second half of the cycle, stimulating sebum. Many women notice jawline and chin breakouts in the week before their period.
- Perimenopause — oestrogen levels decline and become erratic, while androgens remain relatively elevated. The resulting hormonal imbalance drives the menopausal acne surge many women experience in their 40s.
- Stress — cortisol stimulates androgen production. A high-stress week often shows up on the skin a few days later.
- Polycystic ovary syndrome (PCOS) — characterised by elevated androgens, PCOS is one of the most common causes of persistent adult acne in women.
Why You're Still Breaking Out as an Adult
If you're in your 20s, 30s, or 40s and still experiencing acne, the most common underlying factors are:
- Hormonal imbalance — either a clinical condition like PCOS or the natural hormonal shifts of the menstrual cycle and perimenopause
- Gut dysbiosis — an imbalanced microbiome that promotes systemic inflammation and disrupts hormone regulation
- Blood sugar instability — high-glycaemic foods drive insulin spikes, which in turn trigger androgen release
- Nutrient deficiencies — zinc, vitamin A, and vitamin D deficiencies are all linked to impaired skin barrier function and increased acne severity
- Skincare mismatch — products that are too harsh or comedogenic for your skin type can exacerbate underlying issues
- Stress and sleep deprivation — both elevate cortisol and compromise gut barrier function
Understanding which factor is primary for you is the starting point for a targeted approach.
Skin Purging vs Breakouts: Knowing the Difference
Before trying any new skincare or supplement approach, it helps to understand the difference between skin purging — a temporary increase in breakouts caused by increased cell turnover from a new product — and a genuine breakout reaction.
Purging is a normal, time-limited response to active ingredients like retinoids, AHAs, and BHAs. Breakouts triggered by a new product that is wrong for your skin behave differently: they appear in new locations, don't resolve within four to six weeks, and include types of spots (whiteheads, cysts) you don't normally get.
→ Read the full guide: Skin Purging vs Breaking Out: How to Tell the Difference
What's Really Causing Your Adult Acne
For most adults, persistent breakouts have more than one driver. The gut-acne connection is increasingly well-supported — studies have found that adults with acne show significantly different gut microbiome compositions compared to those with clear skin, with lower diversity and reduced populations of Lactobacillus and Bifidobacterium species.
Diet plays a central role. The evidence is now fairly consistent that high-glycaemic diets, dairy (particularly skimmed milk), and ultra-processed foods are associated with acne severity. The mechanism links back to insulin, IGF-1, and androgen signalling.
→ Read the full guide: What's Really Causing Your Adult Acne (Hint: It Starts in Your Gut)
Clearing Hormonal Acne: An Inside-Out Approach
Topical skincare has an important role to play — retinoids, niacinamide, and salicylic acid all have strong evidence behind them. But for hormonal and gut-linked acne, topical treatment alone rarely delivers lasting results. The most sustainable approach combines:
- Dietary adjustments — reducing high-GI foods, dairy, and processed sugar while increasing fibre, fermented foods, and anti-inflammatory nutrients
- Gut microbiome support — targeted probiotics (particularly Lactobacillus and Bifidobacterium strains) and prebiotic foods
- Key supplements — zinc, vitamin D, and omega-3s have the strongest evidence for acne
- Stress and sleep management — often underestimated in their contribution to hormonal breakouts
- Considered skincare — active but gentle, matched to your skin's current condition
→ Read the full guide: How to Clear Hormonal Acne from the Inside Out
A Real-Life Perspective
For many women, acne isn't just a physical issue — it carries real emotional weight. The most honest accounts of clearing hormonal skin describe a process that took months, involved multiple adjustments, and only started working when gut health became part of the picture.
→ Read: My Hormonal Acne Cleared Up When I Fixed My Gut — Here's Exactly What I Did
Supplements with the Strongest Evidence for Acne
If you're looking to support skin health from within, the most evidence-backed options are:
Zinc is arguably the most studied supplement for acne. It inhibits C. acnes, reduces sebum production, and has anti-inflammatory properties. Several randomised controlled trials have found zinc supplementation (particularly zinc gluconate and zinc acetate) comparably effective to tetracycline antibiotics for mild to moderate acne. Standard doses in studies range from 30–45mg elemental zinc daily.
Vitamin D deficiency is significantly more prevalent in people with acne than in the general population. Vitamin D regulates immune responses and has antimicrobial activity. Supplementation at 1,000–4,000 IU daily (depending on baseline levels) is worth exploring, especially in the UK and northern Europe.
Omega-3 fatty acids reduce inflammatory signalling throughout the body. A 2012 randomised trial found that omega-3 supplementation significantly reduced both inflammatory and non-inflammatory acne lesions over 10 weeks.
Probiotics — both oral and topical — are an active area of research. Oral Lactobacillus and Bifidobacterium strains have shown reductions in acne lesion counts in several small trials, with the proposed mechanism being modulation of gut-driven systemic inflammation.

Skincare Ingredients Worth Knowing
For hormonal and gut-linked acne, the most evidence-supported topical ingredients are:
- Retinoids (adapalene, tretinoin) — increase cell turnover, prevent pore blockages, reduce inflammation. The gold standard for acne.
- Niacinamide (vitamin B3) — reduces sebum production, strengthens the skin barrier, anti-inflammatory.
- Salicylic acid (BHA) — oil-soluble, penetrates pores, effective for blackheads and comedonal acne.
- Azelaic acid — anti-inflammatory and antibacterial, gentler than retinoids, good for sensitive or hyperpigmented skin.
- Benzoyl peroxide — kills C. acnes directly; effective but drying — use targeted rather than all-over.
What to avoid for hormonal acne: heavy occlusive moisturisers, fragrance-heavy products, and anything that strips the skin barrier (over-exfoliation is extremely common and significantly worsens hormonal acne).
FAQ
Is hormonal acne the same as regular acne? Hormonal acne refers specifically to breakouts driven by hormonal fluctuations — particularly androgens. It tends to appear in predictable locations (lower face, jaw, chin, neck) and follows cyclical patterns. It's a subset of acne, not a separate condition, but it requires a different treatment approach to acne driven purely by external factors.
Does diet really cause acne? The evidence has strengthened considerably in recent years. High-glycaemic foods, cow's milk (particularly skimmed), and ultra-processed foods are the most consistently associated dietary triggers. Elimination isn't necessary for everyone, but reducing these foods is a reasonable first step and often produces visible results within four to eight weeks.
How long does it take to see results from an inside-out approach? Skin turnover takes around 28 days, and gut microbiome changes take a similar timeframe to stabilise. Most people see meaningful improvement after six to twelve weeks of sustained dietary and supplement changes. Topical results from retinoids typically appear around the 12-week mark.
Can probiotics help with acne? The evidence is preliminary but promising. Several small trials have shown reductions in acne lesion counts with oral Lactobacillus and Bifidobacterium supplementation. The effect appears to be mediated through reduced systemic inflammation rather than any direct action on the skin.
Should I see a dermatologist? For moderate to severe acne, particularly cystic or nodular breakouts, or acne that is causing significant psychological distress, yes — a dermatologist can prescribe treatments (topical retinoids, oral contraceptives, spironolactone, or isotretinoin) that go well beyond what OTC approaches can achieve.
What causes menopausal acne specifically? As oestrogen declines during perimenopause and menopause, androgens become relatively dominant. Sebaceous glands become more sensitive to androgens with age, and the gut microbiome also shifts — further disrupting the hormonal balance that kept skin clear in earlier life.
Is skin purging a sign that a product is working? Purging indicates increased cell turnover, which is a sign that actives are working — but it doesn't guarantee results. If purging lasts longer than six weeks or produces new types of spots, the product may not be right for your skin.
Can stress really cause acne? Yes. Cortisol from stress directly stimulates sebum production and androgen release. Stress also disrupts gut barrier function and sleep — both of which have downstream effects on skin. Many people notice a direct correlation between high-stress periods and skin flare-ups.
Are zinc supplements safe for long-term use? Zinc at doses up to 40mg elemental daily is generally considered safe for most adults. Higher doses (used in some acne studies) should be time-limited or medically supervised, as excess zinc can interfere with copper absorption and cause gastrointestinal side effects.
What's the difference between the gut-skin axis and the gut-brain-skin axis? The gut-skin axis refers to the bidirectional relationship between gut health and skin health. The gut-brain-skin axis extends this to include psychological stress as a mediator — stress disrupts the gut, which disrupts the skin. All three are connected, which is why stress management is a legitimate part of acne treatment.
All Skin Health Guides
→ Skin Purging vs Breaking Out: How to Tell the Difference
→ What's Really Causing Your Adult Acne (Hint: It Starts in Your Gut)
→ How to Clear Hormonal Acne from the Inside Out
→ My Hormonal Acne Cleared Up When I Fixed My Gut — Here's Exactly What I Did
