How Does the Gut-Brain Axis Work?
The gut-brain axis operates through four simultaneous channels: the vagus nerve (80–90% of signals travel gut-to-brain), the enteric nervous system, the HPA stress axis, and immune/metabolic pathways.…
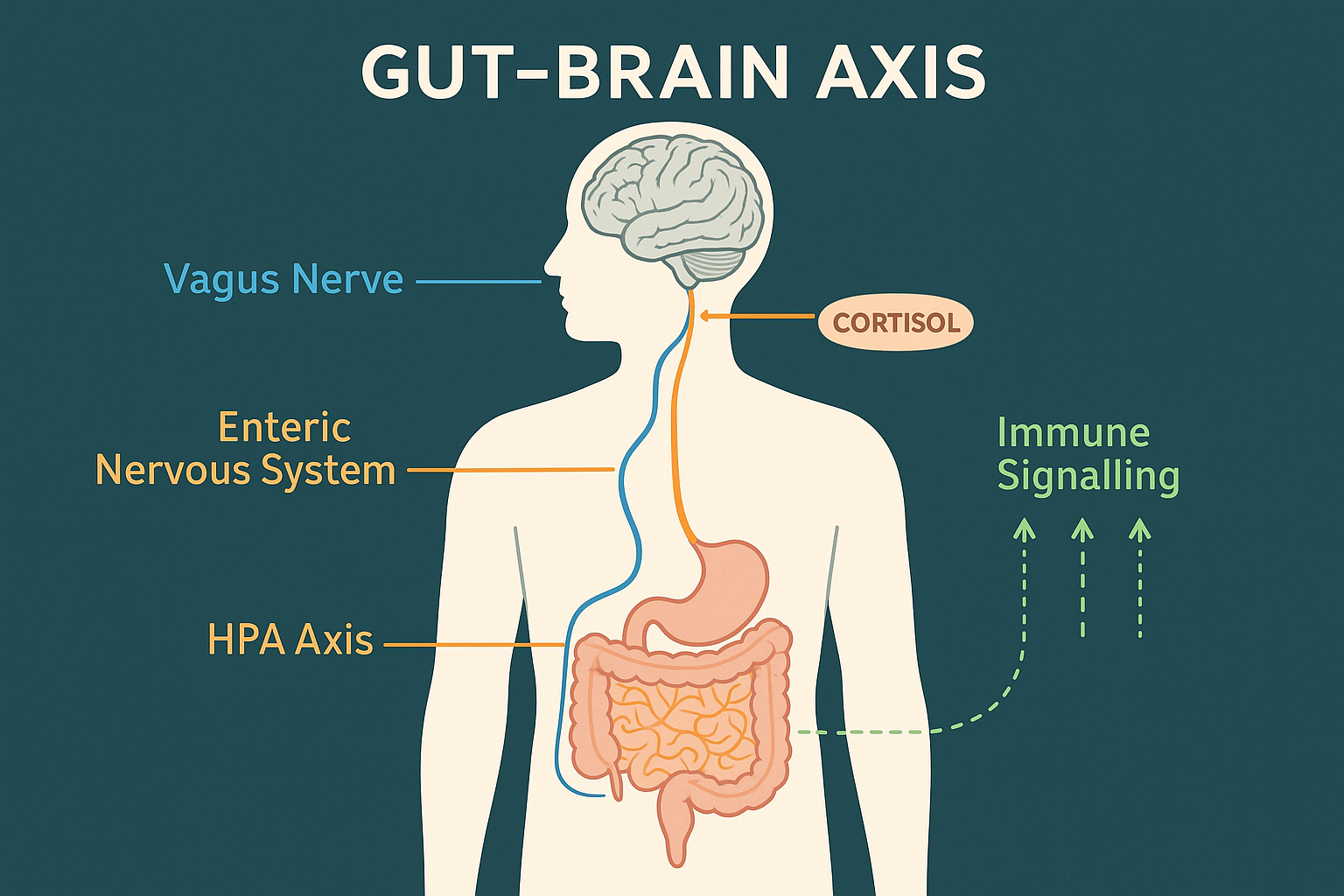
The gut-brain axis operates through four simultaneous bidirectional communication channels: the vagus nerve (direct neural signalling carrying ~500 million signals daily, 80–90% travelling gut-to-brain), the enteric nervous system (500 million gut neurons operating semi-autonomously), the hypothalamic-pituitary-adrenal axis (cortisol and stress response calibration), and immune-metabolic pathways (bacterial metabolites and cytokines crossing the blood-brain barrier). Gut bacteria directly produce serotonin, GABA precursors, and short-chain fatty acids that influence brain function and emotional regulation.
The gut-brain axis works through four simultaneous communication channels connecting your gastrointestinal microbiome to your central nervous system. These pathways operate in parallel and in both directions — the gut continuously sends signals to the brain, and the brain continuously modulates gut function. The net result is that your mental state and your digestive health are in constant biochemical conversation.
The Short Answer
The gut communicates with the brain primarily via the vagus nerve — a direct neural highway that transmits approximately 500 million signals per day, with 80–90% travelling upward from gut to brain. Simultaneously, gut bacteria produce neuroactive molecules (serotonin, GABA, short-chain fatty acids) that enter the bloodstream and cross the blood-brain barrier, influencing mood, cognition, and stress response. The gut also regulates the body's cortisol system and modulates neuroinflammation through immune signalling pathways.
The Science Behind It
Channel 1 — The Vagus Nerve. The vagus nerve runs from the brainstem through the chest and abdomen, innervating the entire digestive tract. It is the fastest communication channel in the gut-brain axis. Specialised sensory cells in the gut lining called neuropods synapse directly with vagal nerve endings, transmitting information about microbial activity, gut wall tension, and luminal chemistry to the brainstem within milliseconds. From there, signals reach the limbic system (emotion), prefrontal cortex (decision-making), and hypothalamus (stress and hormonal regulation).
Channel 2 — The Enteric Nervous System. The gut contains over 500 million neurons — more than the spinal cord — forming the enteric nervous system (ENS), sometimes called the "second brain." The ENS can operate independently of the central nervous system, controlling digestion autonomously. It communicates bidirectionally with the brain via the vagus nerve and spinal afferents.
Channel 3 — The HPA Axis. The hypothalamic-pituitary-adrenal axis governs cortisol secretion in response to stress. Gut bacteria calibrate the sensitivity of this system. Germ-free mice (raised without any microbiome) show exaggerated HPA responses to mild stressors — two to three times the cortisol of normally colonised mice — which normalises when they receive a microbiome transplant. In humans, lower microbial diversity is associated with higher cortisol awakening response and greater perceived stress reactivity.
Channel 4 — Immune and Metabolic Pathways. Gut bacteria produce short-chain fatty acids (butyrate, propionate, acetate) by fermenting dietary fibre. These SCFAs cross the blood-brain barrier, regulate microglial activity (the brain's immune cells), support neurogenesis in the hippocampus, and reduce neuroinflammatory signalling. When gut barrier integrity is compromised, bacterial lipopolysaccharides (LPS) enter circulation and trigger pro-inflammatory cytokines (IL-6, TNF-alpha) that activate brain threat-response pathways — a mechanism implicated in both depression and anxiety.
What This Means For You
Because the gut-brain axis is bidirectional, both gut-targeted and brain-targeted interventions can improve the system. Dietary changes (increasing fermented foods, prebiotic fibre, polyphenol-rich foods) directly modify the microbial signals the gut sends to the brain. Stress-reduction practices (mindfulness, exercise, sleep improvement) reduce the brain's disruptive signals to the gut. The most effective strategies typically address both sides simultaneously.
For the full deep-dive, see The Gut-Brain Axis: How Your Microbiome Controls Your Mood and the comprehensive Gut Health & Mental Wellbeing topic hub.
Related Questions
How long does gut-to-brain signalling take? Vagal signalling operates within milliseconds for direct neural transmission. Hormonal signalling (cortisol, serotonin via circulation) operates on a timescale of minutes to hours. Epigenetic and compositional changes to the microbiome affecting brain function occur over weeks to months.
Is the gut-brain axis the same as the enteric nervous system? No — the enteric nervous system (ENS) is one component of the gut-brain axis, specifically the neural network within the gut wall. The gut-brain axis is the broader system encompassing the ENS, vagus nerve, HPA axis, and immune-metabolic pathways collectively.
Can damage to the vagus nerve affect the gut-brain axis? Yes — vagotomy (surgical severing of the vagus nerve) eliminates many gut-brain signalling effects, as demonstrated in animal studies. Reduced vagal tone — measured via heart rate variability — has been associated with lower microbiome diversity and greater anxiety in human studies.
