7 Signs Your Gut Health Is Affecting Your Mood
Seven clinically-grounded signs that your gut-brain axis may be contributing to mood or anxiety issues: mood shifts after ultra-processed foods, post-antibiotic mood changes, bloating with brain fog, declining stress tolerance, persistent low mood without clear triggers, sleep-mood co-fluctuation,…
The clearest signs that gut health is affecting mood include: anxiety or low mood that worsens after ultra-processed food consumption, persistent bloating co-occurring with heightened stress reactivity, post-antibiotic mood changes, food sensitivities that correlate with brain fog or irritability, morning cortisol spikes with concurrent digestive discomfort, disrupted sleep alongside irregular bowel habits, and mood instability that responds to probiotic or fermented food interventions. These patterns reflect the bidirectional gut-brain axis and are supported by clinical research on LPS translocation, HPA axis dysregulation, and dysbiosis-driven neuroinflammation.
The gut-brain axis is bidirectional — your gut influences your brain and your brain influences your gut. Most people are familiar with gut symptoms triggered by stress: the stomach knot before a difficult conversation, the IBS flare during an anxious period. Less recognised is the reverse: the way chronic gut dysfunction quietly shapes mood, anxiety levels, and cognitive clarity from the inside out.
These signs do not mean your gut is the only cause of low mood or anxiety. But they suggest the gut-brain connection may be contributing — and that addressing gut health could be a meaningful part of the picture.
1. Your Mood Reliably Shifts After Certain Foods
If you notice mood changes — irritability, brain fog, heightened anxiety, or low energy — in the hours after eating specific foods, your gut microbiome may be generating inflammatory signals in response to those foods.
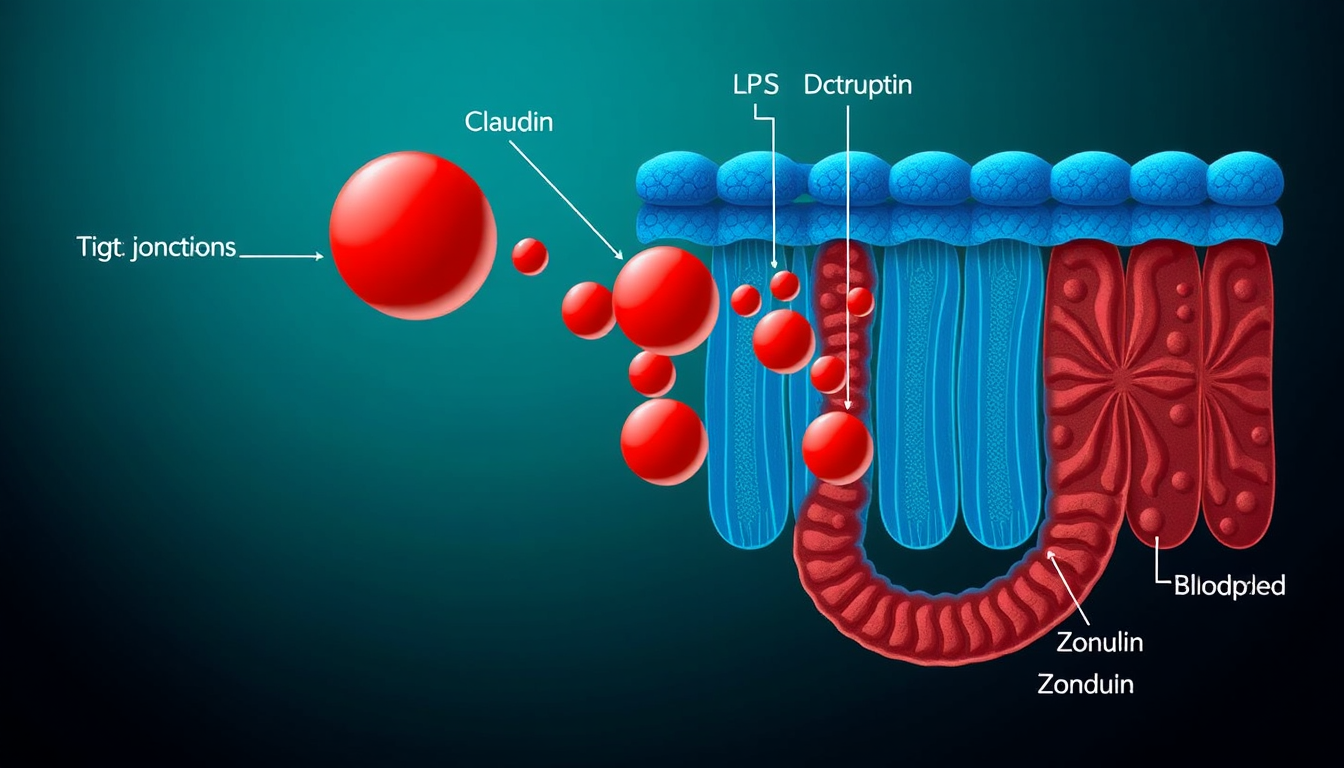
Ultra-processed foods (high in emulsifiers such as polysorbate 80 and carboxymethylcellulose) damage the mucus layer of the gut epithelium, increasing the passage of bacterial lipopolysaccharides (LPS) into the bloodstream. Circulating LPS triggers pro-inflammatory cytokines that cross the blood-brain barrier and activate the brain's immune response within hours. This biological sequence is fast enough to produce same-day mood effects in people with already-compromised gut barriers.
A 2023 study in The British Journal of Psychiatry found that each 10% increase in ultra-processed food as a proportion of diet correlated with a 12% higher odds of clinically significant anxiety symptoms. If your mood tracks closely with diet quality, that's signal worth noting.
2. Anxiety or Low Mood Followed a Course of Antibiotics
Broad-spectrum antibiotics can reduce gut microbial diversity by up to 30%, with some effects persisting for months or years. Lactobacillus and Bifidobacterium species — the primary producers of GABA and key regulators of HPA axis sensitivity — are particularly vulnerable to antibiotic depletion.
If you noticed mood changes, increased anxiety, or emotional blunting that began during or shortly after an antibiotic course, the timing is unlikely to be coincidental. The gut-brain connection disrupted by antibiotics is well-documented. Research published in Gut has shown that the microbiome alterations from a single antibiotic course can shift tryptophan metabolism toward the kynurenine pathway — reducing serotonin precursors — for extended periods.
3. Bloating Correlates With Brain Fog or Irritability
Bloating and distension are symptoms of dysbiosis and altered gut motility — states in which microbial imbalance produces excess fermentation gases and impairs the tight junction proteins that maintain the gut barrier. The same underlying gut conditions that cause bloating (particularly overgrowth of gas-producing bacteria) are also associated with elevated intestinal permeability and systemic LPS exposure.
If you find that your worst mental clarity days coincide with your worst bloating days — not just as a consequence of discomfort, but as a pattern — this gut-brain co-occurrence pattern is consistent with the neuroinflammatory model of gut-driven cognitive impairment.
4. You Are More Stress-Reactive Than You Used to Be
Gut bacteria calibrate the hypothalamic-pituitary-adrenal (HPA) axis — the system governing cortisol release in response to stressors. Germ-free animal studies show that mice with no gut microbiome exhibit cortisol responses two to three times higher than normally colonised mice in response to mild stressors. In humans, lower microbial diversity correlates with higher morning cortisol awakening response and greater self-reported stress reactivity (Psychoneuroendocrinology, 2020).
If your stress tolerance has declined — if things that previously felt manageable now feel overwhelming — and this change has occurred alongside changes to your diet, antibiotic use, or digestive health, a dysbiosis-driven HPA axis shift may be contributing. The gut doesn't just react to stress; it sets the threshold at which stress overwhelms you.
5. You Have Persistent Low Mood With No Clear Psychological Trigger
Major depressive disorder involves dysregulated serotonin, reduced hippocampal neurogenesis, and elevated neuroinflammation — all of which can be driven, at least in part, by gut axis dysfunction. A 2022 meta-analysis in Translational Psychiatry found significantly elevated plasma LPS-binding protein in patients with major depressive disorder compared to controls.
This does not mean that gut dysbiosis is the cause of depression. But if low mood is persistent, treatment-resistant, or accompanied by gut symptoms (IBS, bloating, irregular bowel habits), the LPS-neuroinflammation pathway is a biologically plausible contributor that is often underinvestigated in standard care.
For the specific mechanism linking gut permeability to depression, see Can Leaky Gut Cause Depression?
6. Your Sleep and Mood Fluctuate Together
The gut microbiome has its own circadian rhythm. Disrupted sleep desynchronises microbial activity, reducing short-chain fatty acid (SCFA) production — particularly butyrate, which has documented neuroprotective effects — and increasing inflammatory markers. Conversely, gut dysbiosis impairs melatonin precursor availability (tryptophan metabolism is gut-bacteria-dependent) and disturbs the circadian regulation of gut motility.
Poor sleep and low mood are so tightly correlated that it can be difficult to separate cause from consequence. When that pattern co-occurs with chronic digestive issues or significant dietary changes, the gut-sleep-mood loop is a meaningful piece of the picture.
7. Fermented Foods or Probiotics Noticeably Affect How You Feel
If you have experimented with fermented foods (kefir, kimchi, yoghurt with live cultures) or taken a probiotic supplement and noticed a meaningful shift in anxiety levels, mood stability, or stress tolerance within 4–8 weeks, that response is itself informative. It suggests your gut-brain axis was dysregulated in a way that responded to microbial input — which means the gut-to-brain pathway was influencing your baseline emotional state.
This is not conclusive — placebo effects are real, and individual probiotic responses vary considerably. But a consistent positive response to gut-targeted interventions across multiple attempts is meaningful signal.
What to Do With This Information
These signs are patterns to notice, not diagnoses. If several apply to you, it is worth exploring gut health as a contributing variable — not as a replacement for addressing psychological, social, or pharmaceutical dimensions of mood and anxiety, but as a modifiable biological factor.
The most evidence-supported starting interventions are: removing ultra-processed foods, increasing dietary fibre diversity (targeting 30+ different plant foods per week), incorporating fermented foods daily, and considering a targeted probiotic protocol with clinical evidence for mood outcomes.
For specific foods, see Best Foods for Gut Health and Mental Wellbeing. For a practical meal framework, see The Gut-Brain Diet: A 7-Day Eating Plan for Mental Wellbeing. For the full science of how the gut and mood are connected, see The Gut-Brain Axis: How Your Microbiome Controls Your Mood and the Gut Health & Mental Wellbeing hub.
Frequently Asked Questions
Q: Can gut problems cause depression and anxiety? Yes — gut dysbiosis and intestinal hyperpermeability can contribute to depression and anxiety through the LPS-neuroinflammation pathway, HPA axis dysregulation, and disruption of GABA and serotonin precursor production. These are one set of contributing factors among many; gut health is rarely the sole cause but can be a significant and addressable variable.
Q: How do you know if your gut is causing anxiety? There is no single diagnostic test in routine clinical practice. The clearest indicators are: mood and anxiety patterns that track with diet quality or digestive symptoms, onset of mood changes following antibiotics or significant dietary shifts, and positive mood response to sustained gut-targeted interventions (fermented foods, prebiotics, probiotics) over 4–8 weeks.
Q: What gut tests are relevant for mood problems? In research settings, elevated plasma LPS-binding protein (LBP), intestinal fatty acid binding protein (I-FABP), and low Lactobacillus/Bifidobacterium counts on stool microbiome analysis are the most relevant markers. These are not standard clinical tests. Calprotectin (stool inflammation marker) is more widely available but measures gut inflammation rather than permeability or dysbiosis specifically.
