What Is Cortisol? Functions, Levels & Health
Cortisol is far more than a stress hormone. Learn what it does, how your body controls it, and what high or low levels mean for your health.
Your body is running a remarkably complex balancing act right now — and cortisol is one of its most powerful conductors. Most people only hear about cortisol in the context of stress, burnout, or weight gain. But this hormone does far more than respond to a bad day at work. It regulates your blood sugar, blood pressure, immune response, and even the rhythm that wakes you up each morning.
Understanding cortisol means understanding one of the most influential chemicals in your entire body. Whether your levels are too high, too low, or just right, cortisol has a direct impact on how you feel, function, and recover.
What Is Cortisol and Where Does It Come From?
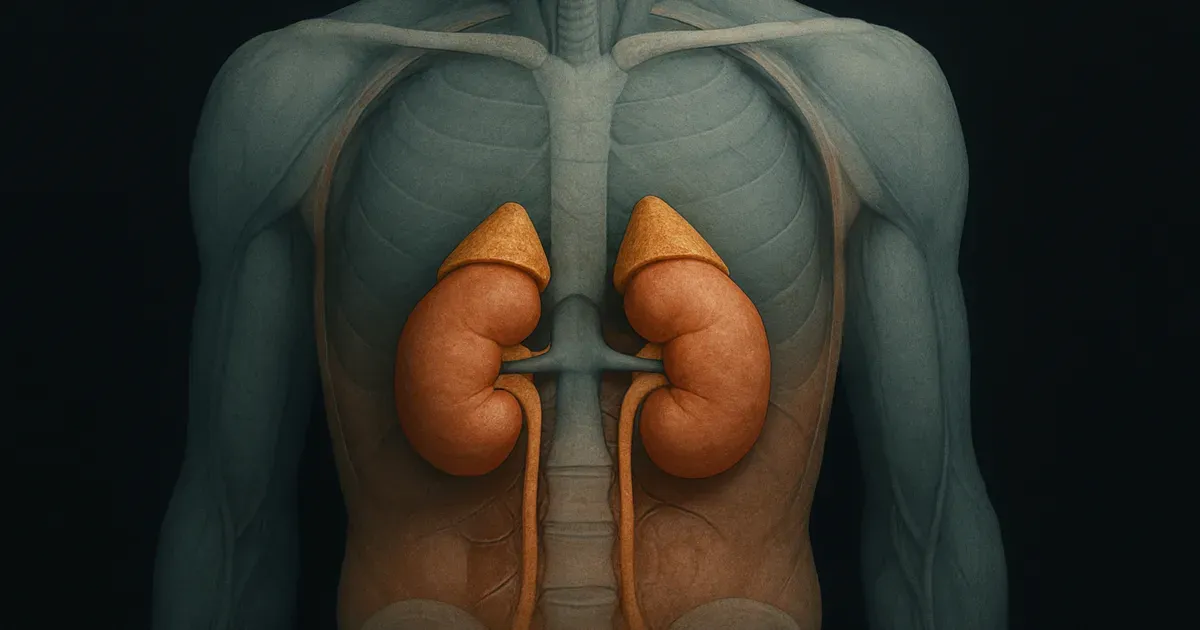
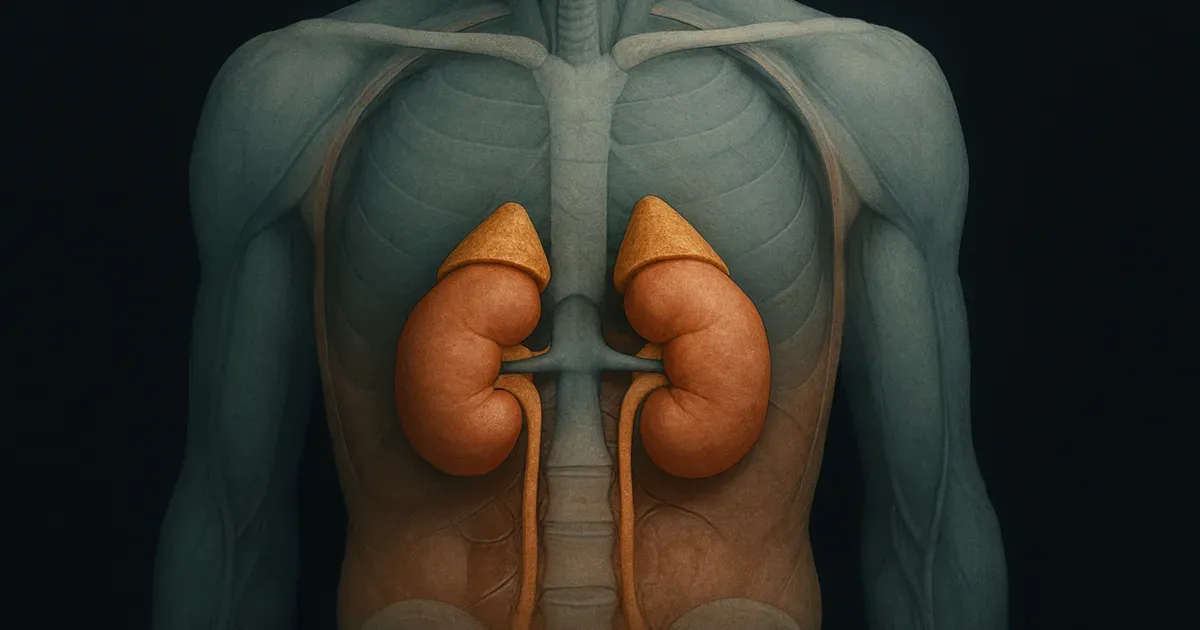
Cortisol is a glucocorticoid hormone produced and released by your adrenal glands — two small, triangular glands that sit on top of your kidneys. As a steroid hormone, it is built from cholesterol and travels through the bloodstream to exert its effects on nearly every organ and tissue in the body.
The production of cortisol is tightly controlled by a feedback loop involving three key players:
- The hypothalamus — detects falling cortisol and releases corticotropin-releasing hormone (CRH)
- The pituitary gland — responds to CRH by releasing adrenocorticotropic hormone (ACTH)
- The adrenal glands — respond to ACTH by producing and releasing cortisol
When cortisol levels rise high enough, this loop switches off — like a thermostat cutting the heat. If any part of this system malfunctions, cortisol levels can spiral too high or sink too low, both of which carry serious health consequences.
The Many Roles Cortisol Plays in Your Body
Cortisol is far more than a stress hormone. It is an essential regulator of multiple bodily systems, working continuously in the background whether you are stressed or completely relaxed. Here is what it actually does:
1. Manages Your Stress Response
When you face stress — whether acute, chronic, or traumatic — your body first releases adrenaline and other "fight or flight" hormones. Cortisol follows, sustaining the alert state and triggering the release of glucose from your liver. That glucose gives your muscles and brain rapid fuel to handle the threat.
This is an ancient, life-preserving mechanism. The problem arises when stress is relentless and cortisol release never fully switches off.
2. Regulates Blood Sugar and Metabolism
Metabolism is the sum of every chemical process keeping you alive, and cortisol sits at its centre. The hormone signals your pancreas to reduce insulin production and increase glucagon, which collectively raise blood glucose levels to ensure energy is available when needed.
Cortisol also acts directly on muscle, fat, and liver tissue to manage how glucose is stored and used. Chronically elevated cortisol can therefore contribute to insulin resistance and eventually Type 2 diabetes.
3. Controls Inflammation
In short bursts, cortisol is anti-inflammatory — it dampens immune overreactions and helps your body recover from injury or illness. This is why synthetic versions of cortisol, such as prednisone, are used medically to treat inflammatory conditions.
However, when cortisol stays elevated for extended periods, the immune system adapts and becomes desensitised to its signal. The result is paradoxical: chronic high cortisol can eventually promote inflammation and leave you more vulnerable to illness.
4. Regulates Blood Pressure
The exact mechanism by which cortisol influences blood pressure in humans is still being researched. What is clear is that elevated cortisol is associated with high blood pressure (hypertension), while abnormally low cortisol is linked to dangerously low blood pressure. Both extremes can be life-threatening if left unmanaged.
5. Governs Your Sleep-Wake Cycle
Cortisol follows a natural daily rhythm called a diurnal pattern. Levels are at their lowest in the evening as you prepare for sleep, then gradually rise through the night, peaking just before you wake up. This morning surge is part of what makes you feel alert and ready to function.
When this pattern is disrupted — by shift work, poor sleep, or chronic stress — the consequences ripple outward into energy, mood, immunity, and metabolic health.

What Happens When Cortisol Levels Are Too High?
Persistently elevated cortisol is known medically as hypercortisolism, and the condition it most commonly causes is called Cushing syndrome. The main causes include:
- Long-term use of corticosteroid medications such as prednisone, prednisolone, or dexamethasone
- ACTH-producing tumours — most often found in the pituitary gland
- Adrenal gland tumours that independently overproduce cortisol
Symptoms of High Cortisol
High cortisol levels can produce a recognisable cluster of symptoms:
- Weight gain, particularly in the face (moon face) and abdomen
- Fatty deposits between the shoulder blades (buffalo hump)
- Wide, purple stretch marks across the belly
- Muscle weakness in the upper arms and thighs
- High blood sugar, which can progress to Type 2 diabetes
- High blood pressure
- Excessive hair growth (hirsutism) in females
- Weak bones and an increased risk of fractures (osteoporosis)
These symptoms can develop gradually and are sometimes mistaken for other conditions, which is why diagnosis often takes time.
What Happens When Cortisol Levels Are Too Low?
Lower-than-normal cortisol is called adrenal insufficiency (or hypocortisolism), and it comes in two forms:
Primary adrenal insufficiency — most commonly caused by the immune system attacking and damaging the adrenal glands themselves. This is known as Addison's disease. Less commonly, it results from infection or loss of blood supply to adrenal tissue.
Secondary adrenal insufficiency — occurs when the pituitary gland underperforms (hypopituitarism) or develops a tumour, limiting ACTH output and therefore cortisol production. It can also be triggered by abruptly stopping long-term corticosteroid treatment, which suppresses the adrenal glands' ability to produce cortisol independently.
Symptoms of Low Cortisol
Adrenal insufficiency can present with symptoms including:
- Persistent fatigue and muscle weakness
- Low blood pressure, especially on standing (orthostatic hypotension)
- Nausea, vomiting, or abdominal pain
- Unintentional weight loss
- Darkening of the skin (in Addison's disease specifically)
- Salt cravings
- Low blood sugar (hypoglycaemia)
Left untreated, severe adrenal insufficiency can become a medical emergency known as an adrenal crisis.
Cortisol and the Gut-Brain Connection
Cortisol does not operate in isolation from your nervous system. The hypothalamic-pituitary-adrenal (HPA) axis — the system that controls cortisol — is deeply intertwined with the gut-brain axis. Chronic stress and elevated cortisol can alter gut microbiome composition, increase intestinal permeability, and worsen gastrointestinal conditions like IBS.
Conversely, signals from the gut can influence HPA axis activity and cortisol output. This bidirectional relationship means that what happens in your gut has real consequences for your cortisol balance — and vice versa. It is one reason why stress so reliably triggers digestive symptoms.
Frequently Asked Questions About Cortisol
Is cortisol always bad?
No — cortisol is essential for survival. It becomes problematic only when levels are chronically too high or persistently too low. Short-term cortisol release in response to stress is a healthy, adaptive response.
Can you test your cortisol levels?
Yes. Cortisol can be measured through blood, urine, or saliva tests. A healthcare provider will typically assess cortisol at specific times of day, given its natural diurnal variation. Home salivary cortisol tests are also commercially available, though they are best interpreted alongside clinical guidance.
How can you support healthy cortisol levels?
Lifestyle factors have a meaningful impact on cortisol regulation. Regular physical activity, consistent sleep schedules, stress management practices (such as mindfulness or breathing exercises), and a balanced diet all support a healthy HPA axis. Avoiding excessive caffeine and alcohol — both of which can elevate cortisol — is also beneficial.
When should you see a doctor about cortisol?
Contact a healthcare provider if you experience symptoms of Cushing syndrome (unexplained weight gain, stretch marks, muscle weakness, high blood pressure) or adrenal insufficiency (persistent fatigue, low blood pressure, unexplained weight loss, nausea). Both conditions require medical diagnosis and management.

The Bottom Line
Cortisol is one of your body's most essential hormones — not merely a marker of stress, but a master regulator of metabolism, immunity, blood pressure, and sleep. Produced by the adrenal glands under the direction of the hypothalamus and pituitary gland, it operates within a finely tuned feedback loop designed to maintain balance.
When that balance tips too far in either direction — whether through tumours, autoimmune conditions, medication, or unrelenting stress — the health consequences are wide-ranging and serious. Recognising the symptoms of both high and low cortisol, and understanding what drives them, is the first step toward protecting your long-term health.
If something feels persistently off — your energy, weight, blood pressure, or stress resilience — cortisol is worth the conversation with your doctor.
