Human Microbiome Explained: Your Biggest Questions Answered
Science-backed answers to the biggest questions about the human microbiome, gut health, immunity, and the gut-brain axis.
The human microbiome is one of the most researched — and most misunderstood — topics in modern health science. Whether you've heard that gut bacteria outnumber your own cells, or you're wondering what your microbiome has to do with your mood, brain, or immune system, you're not alone. The science is genuinely complex, but it's also profoundly relevant to everyday health decisions. This guide answers the questions people ask most often, drawing on peer-reviewed research to cut through the noise.
Quick Navigation
Do bacteria really outnumber human cells in the body?
What does the human microbiome actually do?
How does the gut microbiome affect the immune system?
What is the gut-brain axis and is it real?
How does the microbiome develop from birth?
What is dysbiosis and why does it matter for gut health?
Can diet and lifestyle change your microbiome?
What diseases are linked to microbiome imbalance?
Do bacteria really outnumber human cells in the body?
The classic "10-to-1" ratio of bacteria to human cells is a myth — but the reality is still remarkable. A landmark 2016 study by Sender, Fuchs, and Milo published in Cell revised this figure dramatically, estimating a near 1:1 ratio of bacterial to host cells in a standard adult human body.
The revised estimate places total bacterial cells at roughly 3.8 × 10¹³, compared with approximately 3.0 × 10¹³ human cells. The ratio varies by individual body composition and fluctuates daily, particularly after a bowel movement.
This correction matters because it reframes how we think about our relationship with microbes. Rather than being vastly "outnumbered," humans live in a tightly balanced partnership with their microbial residents — a relationship that has co-evolved over millions of years.
What does the human microbiome actually do?
The human microbiome performs essential biological functions that the host body cannot fully execute on its own. These include metabolising nutrients, producing vitamins, training the immune system, and maintaining the integrity of gut barrier tissue.
Research published in Science by Lynch and Hsiao (2019) describes microbiomes as "sources of emergent host phenotypes" — meaning that traits we think of as uniquely human are partly microbial in origin. This includes aspects of metabolism, mood regulation, and even social behaviour.
Key microbiome functions include:
- Nutrient processing: Breaking down complex carbohydrates and producing short-chain fatty acids
- Immune modulation: Calibrating inflammatory and anti-inflammatory responses
- Pathogen exclusion: Occupying ecological niches that would otherwise be exploited by harmful bacteria
- Neurotransmitter production: Synthesising compounds like serotonin precursors that influence brain function
These functions explain why microbiome disruption carries consequences far beyond digestive discomfort.
How does the gut microbiome affect the immune system?
The gut microbiome and the immune system are in constant, bidirectional dialogue — each shaping the other throughout a person's lifetime. Research by Maynard et al. (2012) in Nature describes these as "reciprocal interactions" that are fundamental to immune homeostasis.
Germ-free mouse studies have provided some of the clearest evidence for this relationship. Animals raised without any microbial exposure show severely underdeveloped lymphoid tissue, reduced IgA antibody responses, and impaired T-cell differentiation — deficits that can be partially reversed by microbial colonisation.
Specific bacterial species direct the differentiation of IL-17-producing T-helper cells in the small intestine (Ivanov et al., 2008), demonstrating that immune cell identity is partly determined by which microbes are present. Belkaid and Hand (2014) summarise this relationship succinctly: the microbiota helps set the immune system's baseline "tone."
An imbalanced gut microbiome — a state called dysbiosis — has been associated with inflammatory bowel disease, celiac disease, and rheumatoid arthritis, underscoring how central microbial balance is to immune health.
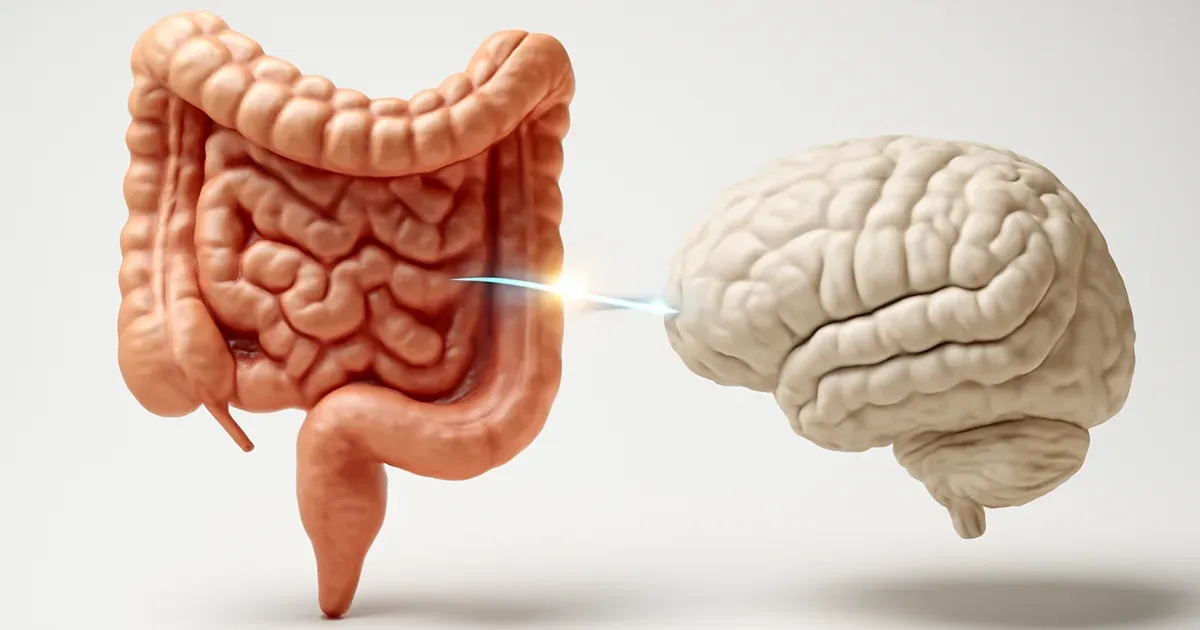
What is the gut-brain axis and is it real?
The gut-brain axis is a scientifically validated, bidirectional communication network linking the gastrointestinal tract and the central nervous system. It operates through neural, hormonal, and immune signalling pathways, and the microbiome plays an active role in all three.
The gut contains roughly 500 million neurons — part of the enteric nervous system — and communicates directly with the brain via the vagus nerve. Gut bacteria influence this signalling by producing neurotransmitter precursors, metabolites, and immune molecules that cross or signal across the blood-brain barrier.
Main and Minter (2017) have explored how microbial immune communication contributes to neurodegenerative diseases, suggesting the gut-brain axis is relevant not just to mood but to conditions like Parkinson's and Alzheimer's disease.
Practical implications of gut-brain axis research include:
- Mood and anxiety: Gut microbiota composition correlates with anxiety-like behaviour in animal models
- Stress response: Dysbiosis can amplify the HPA axis stress response
- Neuroinflammation: Gut-derived inflammatory signals may drive brain inflammation over time
- Cognitive function: Emerging evidence links microbiome diversity to sharper cognitive performance
How does the microbiome develop from birth?
A baby's microbiome begins forming at — or possibly before — birth, and the events of early life have lifelong immunological consequences. Research by Gensollen et al. (2016) in Science establishes that early microbial colonisation fundamentally shapes the developing immune system in ways that persist into adulthood.
Delivery mode is one of the earliest determinants of microbiome composition. Dominguez-Bello et al. (2010) showed that vaginally delivered infants acquire microbial communities resembling the maternal vaginal microbiota, while caesarean-born infants are colonised by skin and environmental microbes instead — a difference that may influence allergy and asthma risk.
The trajectory of infant microbiome development follows a recognisable pattern:
- Birth to 3 months: Dominated by maternal microbes from delivery and breastfeeding
- Introduction of solids: Rapid diversification of bacterial species
- Age 2–3: Microbiome begins to resemble adult composition
- Antibiotic exposure: Early-life antibiotics can disrupt this trajectory, increasing allergy susceptibility (Russell et al., 2012)
Maternal antibodies transferred through breast milk also help protect neonates by targeting specific microbiota-associated pathogens, as demonstrated by Zheng et al. (2020) in Nature.
What is dysbiosis and why does it matter for gut health?
Dysbiosis refers to an imbalance in the composition or function of the microbiome, and it is increasingly recognised as a driver of systemic disease rather than merely a symptom. Belizario et al. (2018) frame gut microbiome dysbiosis as a "new frontier" in understanding and treating metabolic disease.
Dysbiosis can arise from many causes: antibiotic use, poor diet, chronic stress, infections, or disrupted sleep. Once established, it can create a self-reinforcing cycle where a compromised gut barrier allows microbial products to enter the bloodstream, triggering systemic inflammation.
Gut health is directly dependent on microbial balance. When commensal bacteria are depleted, opportunistic pathogens fill the gap, and the immune system loses its well-trained calibration.
| Condition | Microbiome Link | Key Evidence |
|---|---|---|
| Inflammatory Bowel Disease | Reduced microbial diversity | Zhang et al., 2017 |
| Rheumatoid Arthritis | Specific dysbiotic signatures | Maeda & Takeda, 2019 |
| Celiac Disease | Altered duodenal microbiota | Valitutti et al., 2019 |
| Gestational Diabetes | Maternal/neonatal dysbiosis | Wang et al., 2018 |
| Cancer Immunotherapy | Microbiome predicts response | Gopalakrishnan et al., 2018 |
Restoring microbial balance through targeted dietary changes, probiotics, or faecal microbiota transplantation (FMT) is an active area of therapeutic research.

Can diet and lifestyle change your microbiome?
Yes — the human microbiome is highly responsive to diet, and changes can occur within days of a dietary shift. This plasticity is one of the most actionable findings in microbiome science, because it means gut health is genuinely modifiable through everyday choices.
Dietary fibre is the primary fuel source for beneficial gut bacteria. Fermented foods introduce live microbial populations. Polyphenols found in vegetables and fruits act as prebiotics, selectively feeding health-promoting species.
Lifestyle factors that shape microbiome composition include:
- Diet: High-fibre, plant-rich diets associate with greater microbial diversity
- Exercise: Regular physical activity correlates with enriched short-chain fatty acid-producing bacteria
- Stress: Chronic psychological stress alters gut motility and microbial balance
- Sleep: Circadian disruption impairs microbiome rhythmicity
- Medications: Antibiotics, proton pump inhibitors, and metformin all alter microbiome composition
Hacquard et al. (2015) note that the interplay between microbiota and host nutrition is deeply conserved across animal kingdoms — suggesting that feeding your microbiome well is not a modern wellness trend but an evolutionary imperative.
What diseases are linked to microbiome imbalance?
Microbiome imbalance has been credibly linked to conditions spanning the gut, brain, joints, metabolism, and even cancer. The integrative Human Microbiome Project (iHMP), whose findings were published in Nature in 2019, mapped microbiome changes across multiple diseases simultaneously, confirming that dysbiosis is rarely isolated to one organ system.
Gopalakrishnan et al. (2018) found that the gut microbiome influences both cancer development and the effectiveness of immunotherapy treatments — patients with more diverse microbiomes responded significantly better to checkpoint inhibitor drugs.
For neurodegenerative conditions, Main and Minter (2017) documented how disrupted microbial-immune communication may accelerate neuroinflammation. Meanwhile, gestational diabetes has been associated with dysbiosis in both mother and newborn, suggesting the microbiome's influence begins before birth.
The breadth of disease associations does not mean the microbiome causes all of these conditions — but it does mean that microbiome health is a meaningful lever for prevention and treatment strategies across many medical specialities.
Bottom Line
- The human microbiome is a near 1:1 partner with our own cells — not a vast, alien colony living inside us.
- Gut health is immune health: A balanced microbiome trains and regulates the entire immune system from birth onward.
- The gut-brain axis is real and clinically relevant, linking microbial balance to mood, stress response, and neurodegeneration.
- Early life microbiome events have lifelong consequences, from delivery mode to antibiotic exposure in infancy.
- Diet and lifestyle are the most powerful tools available to maintain or restore microbiome balance — and the evidence is robust.
